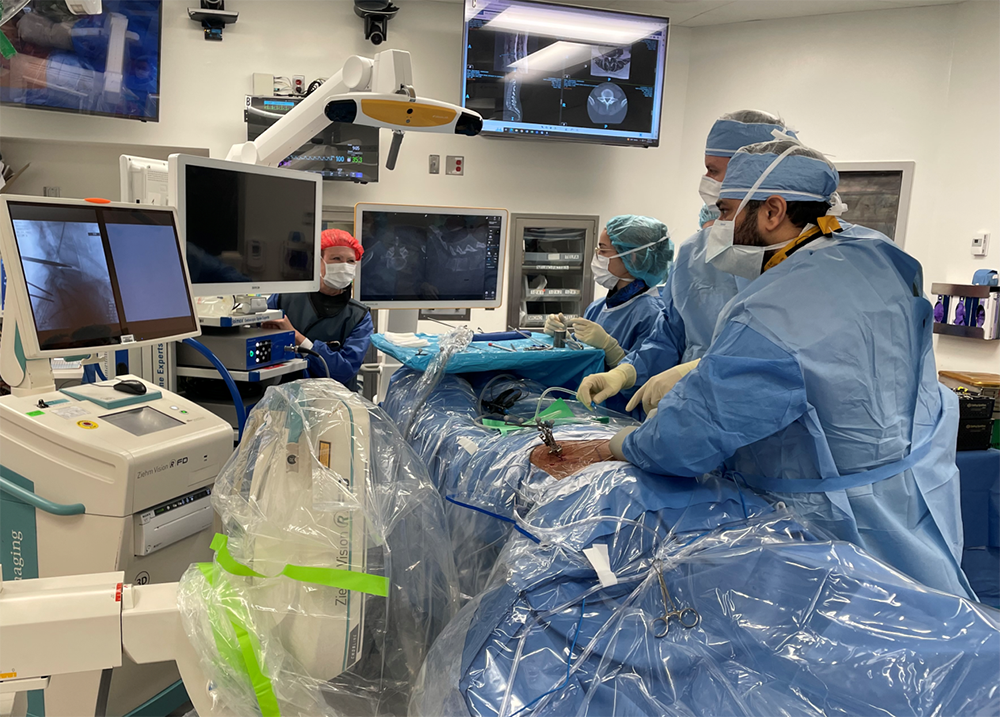
Dr. Ibrahim Hussain achieved a spine surgery milestone when he performed the first 3D navigation-guided endoscopic lumbar fusion (transforaminal lumbar interbody fusion, or TLIF) ever performed in New York City in late 2022, becoming one of the few surgeons in the United States performing this procedure. The surgery was successful, and the patient is doing extremely well.
The endoscopic portion of the case, involving discectomy and placement of a collapsed interbody “cage” that is then bidirectionally expanded once inside the disc space, required an incision only 1 cm long. Pedicle screws were placed separately through similar short incisions. For comparison, traditional open TLIF surgery requires an incision between 3 and 6 inches, with extensive muscle dissection and bleeding, and patients typically require postoperative narcotics. Current minimally invasive techniques for TLIF, which are still very effective procedures for most patients, can reduce the incision to just to 1.5 inches, but still requires bone (facet joint) drilling and resection to achieve similar goals. Endoscopic fusion, however, leverages an oblique trajectory through a natural corridor (Kambin’s triangle) to the disc space without requiring bone drilling, muscle dissection, or excessive nerve manipulation. It reduces the incision to well under an inch and brings a new era of ultra-minimally invasive spine surgery to our patients.
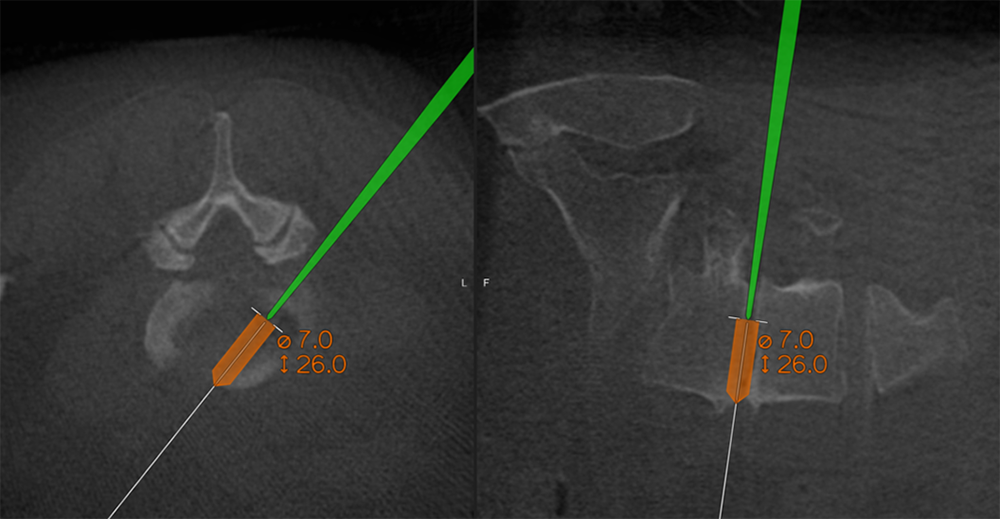
Above: The trajectory is carefully planned using 3D navigation-guided mapping; this step also allows accurate sizing of the implant.
“This is a landmark in spine surgery and shows once again how Weill Cornell Medicine and the NewYork-Presbyterian Och Spine program are leading the way in innovative surgical techniques,” says Dr. Roger Härtl, chief of spine surgery at Weill Cornell Medicine and co-director of NewYork-Presbyterian Och Spine. “We are already leaders in MIS and navigation, and this is another step forward in making complex surgery even less invasive and safer for our patients. Dr. Hussain, along with other surgeons in our endoscopic spine surgery program, are expanding the surgical options for patients who will benefit from the least invasive techniques.”
“As always,” says Dr. Philip E. Stieg, Chairman and Neurosurgeon-in-Chief and Margaret and Robert J. Hariri, MD ’87, PhD ’87 Professor of Neurological Surgery, “with careful patient selection and a focus on safety, symptom relief, and quality, we can advance the field as well as deliver superb outcomes.”
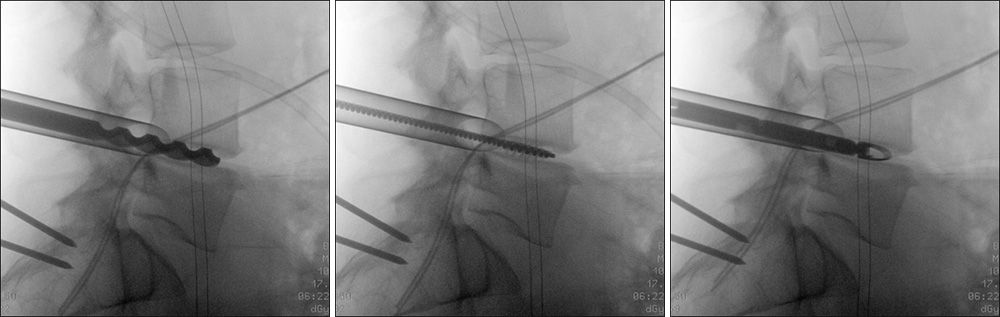
These small-diameter devices are used to complete the discectomy and prepare the endplate for the interbody cage.
Endoscopic spine surgery, which has been evolving since the early 1980s, has witnessed a resurgence in the past decade due to advancement in optical lens and instrumentation technology. It is optimal in a wide spectrum of patients, from those who may not be healthy enough to tolerate open or even minimally invasive techniques (due to age or physical conditions that would rule out extended time under anesthesia) to young and active individuals with disc herniations, spinal stenosis, or instability (affording them the best opportunity to return to activity faster). As spinal endoscopy continues to advance, and as indications broaden with experienced surgeons, it becomes an attractive and effective option for patients of any age or condition, offering the very smallest of incisions, short times under sedation, and quick recoveries with less pain.
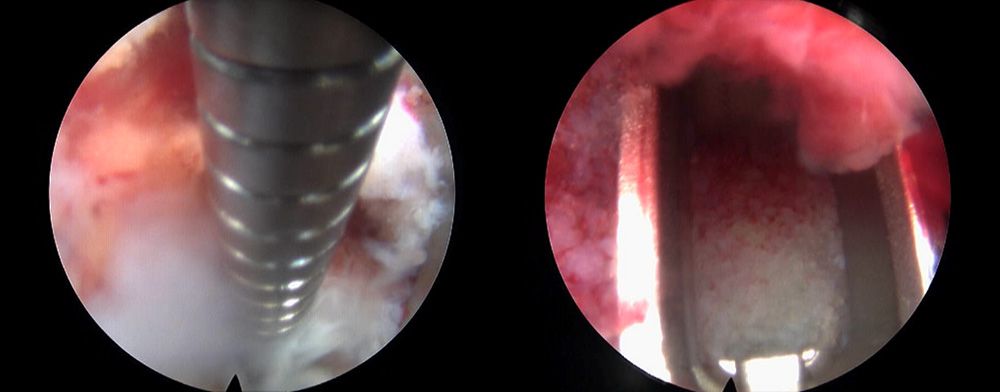
Left: Performing the discectomy and disc preparation using modified extended and flexible instruments designed to fit through the endoscope. Right: A close-up view of the interbody cage after placement and expansion with packed bone graft in the center to facilitate fusion.
Find out more about our endoscopic spine surgery program
See also: Getting Back to Normal: An Endoscopic Spine Story
.